Diagnosing mesothelioma
Diagnosing mesothelioma can be difficult to do if only symptoms are considered.
The reason is that the symptoms of mesothelioma resemble those of many other conditions. Consequently, to produce a definitive mesothelioma diagnosis, doctors utilize one or more advanced medical tests.
However, before they decide which test or tests to administer, doctors almost always request patients fill out a medical history. This is basically a questionnaire in which patients are asked about their current and past health status, lifestyle, employment, hospitalizations, and illnesses that afflicted their parents, siblings, and offspring.
The information supplied to doctors via the medical history questionnaire should alert them either directly or by inference to the patient’s prior exposure to asbestos. If so alerted, that insight should signal to doctors that they need to conduct diagnostic tests specific to mesothelioma.
There are three main categories of mesothelioma diagnostic tests. They are:
- Imaging studies
- Blood screenings or assays
- Biopsies
Results from an imaging study are generally available within a day or two. Results from a blood screening or assay usually take a week or longer. Results from a biopsy—which is considered the most definitive test for mesothelioma—seldom come back from the lab sooner than a month, with waits of 90 days or more the norm.
Mesothelioma imaging studies
One of the imaging technologies most extensively utilized for diagnosing mesothelioma is positron emission tomography (PET).
PET involves placing a tracer solution into the patient’s body and then using a photon scanner to see how much of the tracer is gobbled up by cells.
The tracer is known as a radionuclide. Healthy cells consume little of it. Cancer cells, on the other hand, gorge on it. The imaging camera used in a PET test detects these differing levels of consumption and vividly shows the location of cells that are cancerous.
The PET scan takes about 90 minutes to perform. It begins with the intravenous infusion of the tracer, which is a process that runs about 20 minutes. This is followed by a wait of about 45 minutes to allow the tracer to fully circulate throughout the body. The imaging then begins and continues for roughly the next 25 minutes.
Imaging data collected by the scanner is funneled to a computer which analyzes and translates them into a picture. Finally, a radiologist interprets what the picture reveals. The physician who ordered the test then receives a report from the radiologist and makes its findings known to the patient.
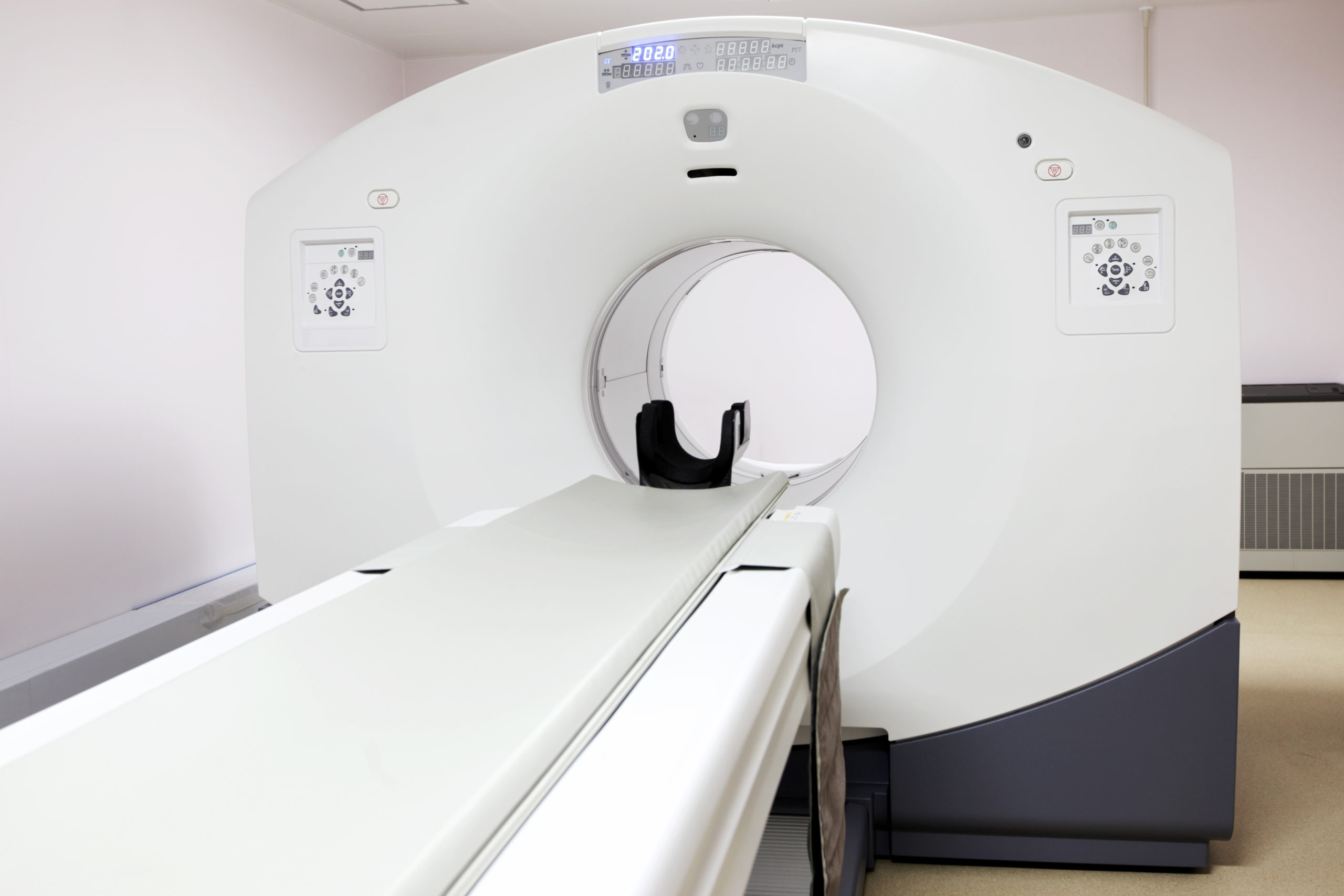
Another extensively used imaging technology for diagnosing mesothelioma is computed tomography (CT). Here, the patient’s body is x-rayed with the resulting imaging data processed through a computer. This permits the showing of far more detail than would be otherwise possible with x-rays alone. CT images also can be generated in three dimensions, which helps doctors better characterize the size and shape of any detected suspicious masses.
Doctors have the option to order CT studies with contrast. For this, the patient is given a liquid—usually administered orally—prior to the study so that the anatomic structures and anomalies picked up by the scanner will stand out in the pictures that are produced.
CT provides diagnostic information that PET cannot, and vice versa. Accordingly, the two tests are often performed together. There even are hybrid machines that combine CT and PET in one system. The combined test is called PET-CT, and it is considered the standard of care for mesothelioma diagnosis.
Mesothelioma blood screenings and assays
Mesothelioma cells leave telltale signs of their presence. The signs are in the form of certain molecules released by the cells as byproducts of their metabolism.
All cells expel metabolic byproducts. However, the ones generated by cancerous cells are different from those of healthy ones. Regardless of whether they come from healthy or diseased cells, the byproducts soon find their way into the bloodstream.
The first step in performing a mesothelioma blood test entails collecting a specimen of blood. It is customarily drawn from a vein in the arm. The specimen is then sent to a lab for assaying. At the lab, technicians test the specimen for the metabolic byproducts, which are known as biomarkers.
The results of blood screenings and assays are useful, but not at this time considered reliable enough to yield a definitive mesothelioma diagnosis. Doctors mainly look to mesothelioma blood tests for confirmation that they are on the right track in suspecting mesothelioma.
Mesothelioma biopsy
The truly definitive test for mesothelioma is a biopsy, a procedure in which a sample of a suspicious mass is surgically extracted for microscopic examination in a lab.
There are different ways a sample can be obtained.
In an excisional biopsy, the doctor uses a surgical knife to open a slit in the chest or abdomen and then remove a sizable piece of the mass (the existence and location of the mass is detected earlier with the aid of an imaging test).
A more common biopsy technique is fine-needle aspiration (FNA). Here, the doctor uses a CT or an ultrasound imaging system to guide the insertion of a thin, syringe-mounted needle into the chest or abdomen. When the needle contacts the targeted mass, the doctor pulls back on the syringe’s plunger to extract little bits of tissue.
Doctors also have the option of merely observing the suspect mass rather than removing samples of it. The procedure for this called a thoracoscopy. It entails the surgical insertion of an endoscope, which is a thin, flexible tube with a tiny video camera mounted at the tip. The camera streams live pictures of the interior of the chest cavity or abdominal cavity, giving a real-time look at the mass.
Another biopsy related option available to doctors is thoracentesis. This is a procedure for extracting pleural fluid from the chest cavity. When pleural mesothelioma onsets, it causes the lining around the lungs to overproduce fluid. Some of the cancer’s cells end up in this fluid and can be detected when a specimen of the fluid is examined under a microscope. Thoracentesis is performed by inserting an imaging-guided needle through the patient’s back; when the needle is properly positioned, a tube is attached to it and the fluid then flows out into a collection vial.
After a mesothelioma diagnosis, talk to a mesothelioma lawyer
Once a doctor makes a definitive diagnosis of mesothelioma, it may be time to consider using the legal system to seek compensation for having developed the disease.
People who develop mesothelioma and who have at some point in their past been exposed to asbestos may be entitled to money from the businesses responsible for causing that exposure.
Likewise, the loved ones of mesothelioma patients may be entitled to compensation.
The best way to begin the process of seeking such money is to contact a lawyer extensively experienced in mesothelioma litigation.
A mesothelioma lawyer can explain the legal rights to compensation that exist for mesothelioma patients and/or their loved ones. Compensation can include money to pay for medical bills and related expenses not covered by insurance. Compensation can also include money to make up for wages lost because of inability to work and to make up for the pain and suffering wrought by the disease.
To talk to a mesothelioma lawyer, click here.

About the author…
Gregory Sandifer graduated from Southern Illinois University Edwardsville and received his law degree from Western State University College of Law in Fullerton, California.